Ever felt like you’re leaving money on the table despite having sophisticated billing systems? That’s the challenge payment integrity aims to solve.
For years, I’ve watched healthcare organizations struggle with overpayments and underpayments, missing crucial opportunities to optimize their revenue. Payment integrity isn’t just another buzzword—it’s a critical function that ensures claims are paid correctly the first time, reducing the need for costly retrospective audits and recovery efforts.
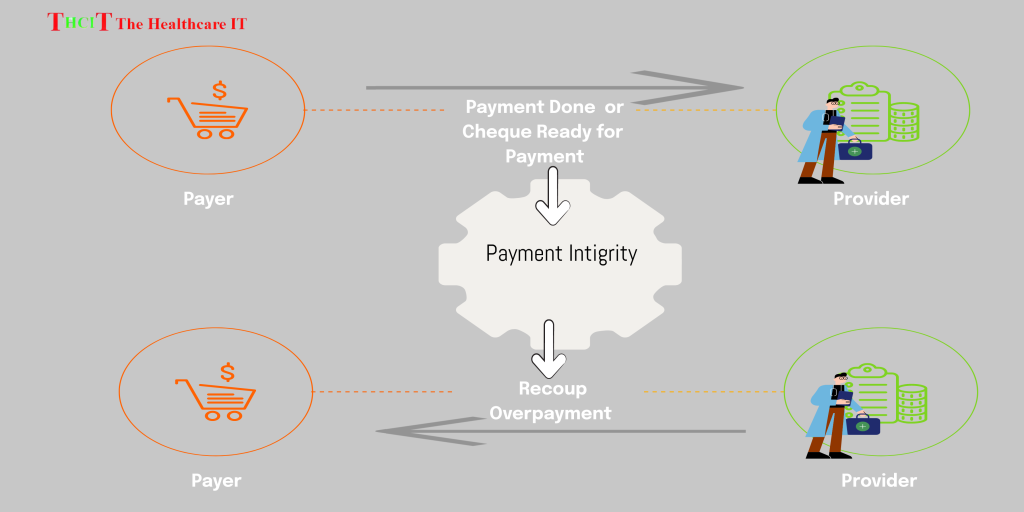
At its core, payment integrity combines clinical knowledge, coding expertise, and data analytics to identify improper payments. For payers, this means finding overpayment opportunities. For providers, it means ensuring they’re not leaving legitimate reimbursement on the table.
The technology powering effective payment integrity solutions has evolved dramatically. Modern systems use rule engines that can process thousands of concepts across multiple programs—from Diagnosis Related Groups (DRG) to Skilled Nursing Facility (SNF) claims to Durable Medical Equipment (DME).
What makes payment integrity particularly challenging is the need to stay current with constantly changing payment policies, coding guidelines, and clinical best practices. This requires a combination of subject matter expertise and sophisticated technology that can adapt quickly to new requirements.
The most effective payment integrity programs don’t just focus on recovering funds—they use the insights gained to improve front-end processes, creating a continuous improvement loop that reduces payment errors over time.
Are payment integrity challenges affecting your healthcare organization? What approaches have you found effective? Share your experiences in the comments below!
#PaymentIntegrity #HealthcareFinance #RevenueCycle


