Revenue cycle management (RCM) is the financial backbone of any practice, ensuring timely reimbursement for services. A good RCM process and technology ensures regular and timely cash flow for healthcare provider businesses.
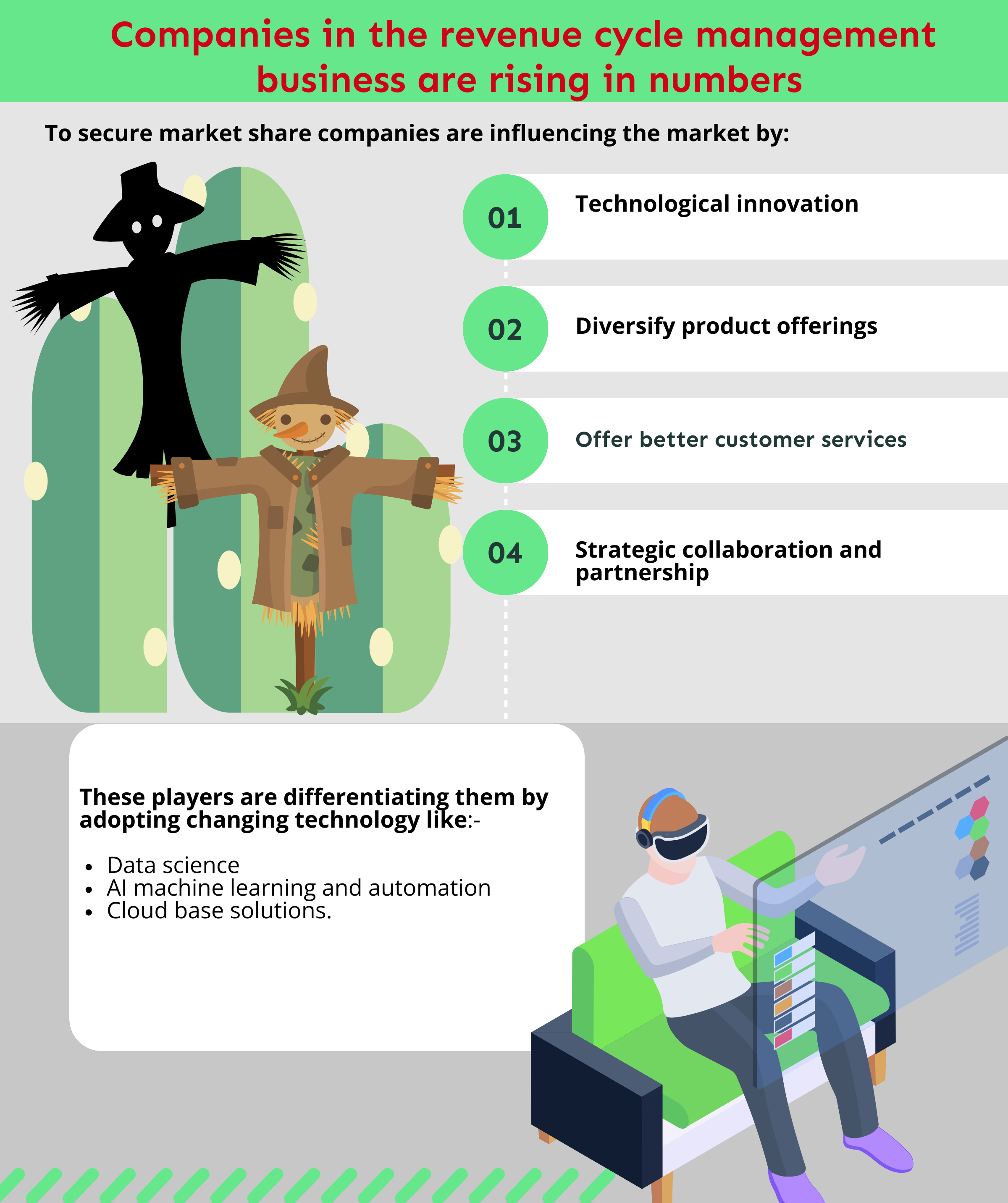
Revenue Cycle Management businesses face ongoing challenges from government and insurance companies that directly or indirectly hit the provider’s bottom line.
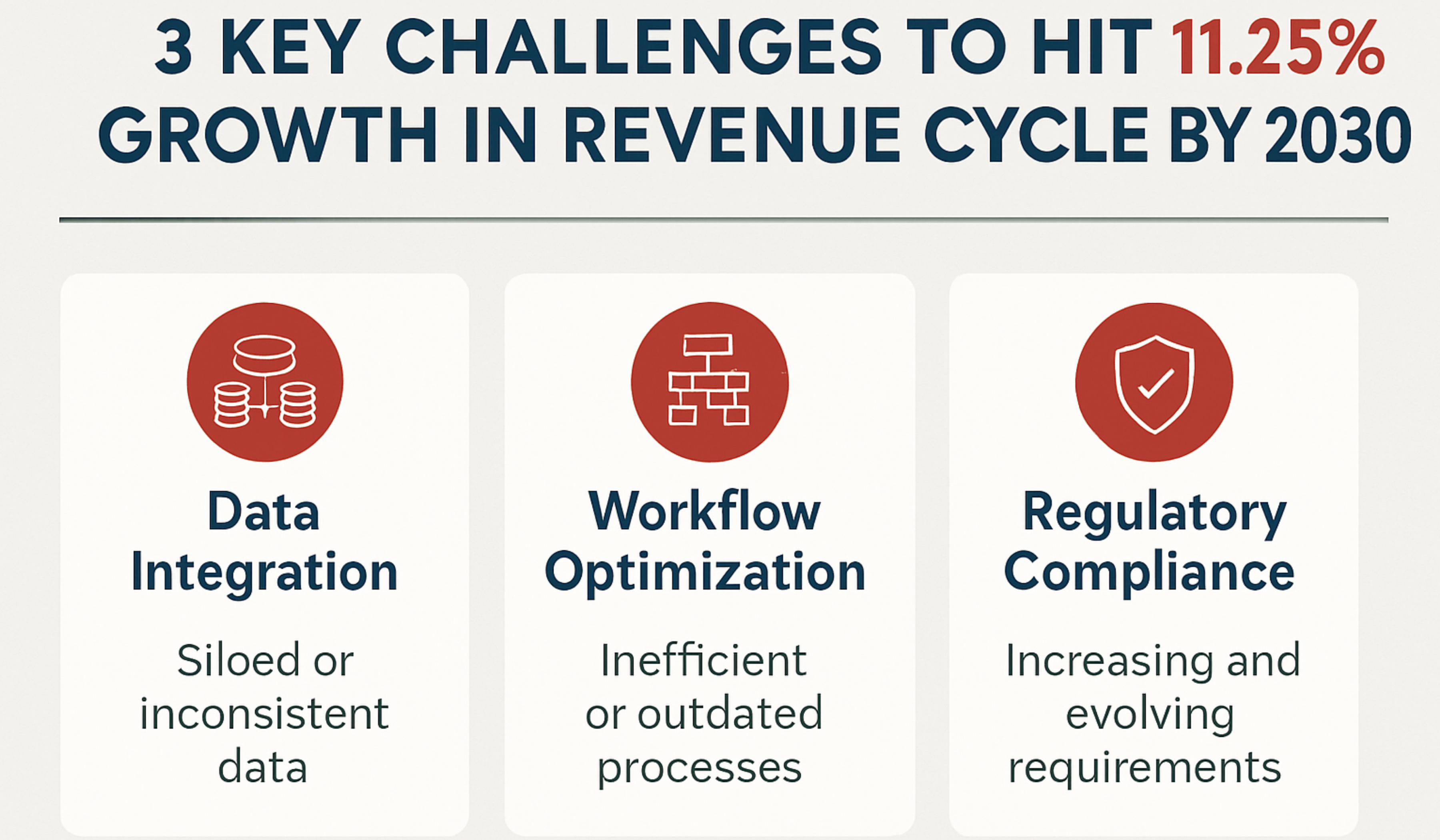
Challenges in RCM business
Lack of visibility in data
A big-picture view in RCM business helps organizations formulate the right strategies and tactical measures to improve revenue for the provider business. The healthcare technology business lacks insights and required data to diagnose problems in revenue cycle management processes.
Disparate systems can be major obstacles in problem-solving and decision-making that would result in slowing down claims, billing, and payment processes. One unified system from the front office through mid-office and back office in a healthcare organization would give complete visibility on each process within the revenue cycle. It is critical to identify, collect, organize, clean data, and have meaningful integration between various systems and data sets.
A data-driven approach would help to identify areas of improvement that can enhance revenue opportunities like optimizing coding practice, improving in denial management process, and improving turnaround time for transactions between provider, payer, and patient.
Complex billing process
The US healthcare medical billing process is the most complex process in the healthcare system. Complexity arises from involvement of multiple stakeholders, strict regulations, Interoperability standards and administrative steps.
Commercial and government insurers like Medicare and Medicaid have different rules, codes, and regulations standards. In the Managed healthcare system billing differs when it comes to In-network or out of network provider for patient insurance. Billing rules may also differ from state to state.
The US healthcare coding system involves more than 70,000 diagnostic codes (ICD 10 – CM) and thousands of CPT (HCPCS (Procedure Codes) with Modifiers. Modifier gives additional information on procedure code like procedure is performed on right or left or both sides of body.
Frequent and Annual regulation changes from CMS (Centers for Medicare and Medicaid Services) and private payers. They also make changes in billing rules. Electronic billing must comply with stringent data privacy and security requirements from HIPAA. Not to forget new rules on surprise billing and price transparency (No Surprises Act (2022) add to the complexity of US medical billing.
High Rate of denials and rejects approx. 10-20% of claims are initially denied due to coding errors incorrect patient, provider, or insurance information, missing prior authorization, or lack of medical necessity. The appeal process is not only costly but also a time-consuming process. Long payment cycles of 30 to 90 days and underpayment to healthcare providers pose challenges to coping with operating expenses for healthcare providers.
High deductibles and copayments often have collection difficulties for patients. Providers also face challenges in settling the balance of payment that arises when patients are billed but they refuse to pay. EOBs (Explanation of Benefit) are confusing, and patients often find it difficult to interpretant this Itemized charges.
Challenges in RCM Automation

Various stakeholders in the US healthcare system have their own software and technology. EHR, Billing Software for provider, Lab and DI software system, Patient Portal and Payer claim adjudication system are various software systems.
Generally, the Provider side communicates using HL 7 and FHIR framework, and EDI transaction framework is used to communicate between healthcare facility and Insurances houses. Nuclear technology stake and framework poses challenge in seamless interoperability, end to end connectivity, flow of information and leverage technology advantages for quality and cost-efficient healthcare services.
High initial cost, fast technology development, and ROI uncertainty is creating immense pressure for healthcare provider businesses. Implementing automation tools like AI, machine learning, robotic processes, IOT, moving to cloud and software tools need high software licenses and infrastructure cost, and it might take years to meet breakeven. In addition, training costs also add overhead to businesses.
Healthcare Providers’ software often run on legacy technology and frameworks. Integration of modern automation tools, Infrastructure and framework are hurdles for adopting new technologies. Lack in proper solution architecting or/and Improper integration causes day-to-day operation loss like inconsistent data, errors, system down issue, or high maintenance cost to fix the ongoing incident.
Automation can be a liability if it does not address data consistency and completeness issues. Quality and accuracy of data are the sole foundation for implementation of Data Analytics and AI tools.
Automation is not only about technology, but it is more about human emotion. Employees fear losing jobs and resistance to change, the low usage rate of implemented technology is always a challenge in the implementation of automation.
Healthcare technology needs to ensure all compliance and security requirements are met. HIPPA, GDPR, and other regulations require strict data security. PHI and PII are required to be protected in every layer of technology. Payers might mandate provider business solution organization to comply with certification like HITRUST and SOC2 to partner to perform business. Cost of technology also go high if technology is required to be hosted and maintained in US by payers or regulation rather than moving to low-cost countries like India or Philippines.
Automation can very well take away a lot of routine day-to-day manual tasks, and complex claim but it still needs certified Nurse, Doctors or certified professional review it causes duplicate effort and delay in resolution.
Different Health Insurance companies have different billing rules and policies. Customization of automation solutions for each payer is a costly affair for provider technology businesses. The maintenance cost of technology goes up when Insurance companies make changes in these billing rules and polices.
Human resource challenges
Companies rendering Revenue Cycle Management (RCM) services are struggling to retain experienced talent. Employees in RCM services have to perform monotonous tasks and are under high pressure to complete tasks in a short timeline.
The medical billing industry has a shortage of certified coders (CPC, CCS) and experienced billers.
Changes in compliance, payer policies, and regulation requires employees to invest time to be updated to prevent claim denial. High pressure of day-to-day operation tasks, force employees to spend extra hours to stay current. Employees are always at risk of penalties due to staff errors.
Due to the increase in competition in the RCM business. RCM services are running with a limited budget for professional development and rewards and recognition. High revenue targets and low budget for training causes reduce morale of work force.
Please comment and let me know the challenges you are facing in RCM Business.